
Dr. Sunita Lawange
Anaesthesiologist, Nagpur
The contemporary era in pain management really began with the discovery of nitrous oxide and its analgesic properties in the late 18th century. This was soon followed by scientific investigation of the anaesthetic properties of nitrous oxide and ether on animals, and the use of these substances in human patients.
Surgical anaesthesia was first publicly demonstrated at Massachusetts General Hospital in 1845 and 1846. The discovery and use of anaesthetics changed the perception of pain (Fig.1)
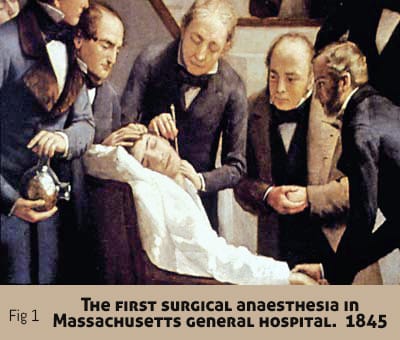
In the 1850s Charles Gabriel Pravaz, a French surgeon, and Alexander Wood of Edinburgh independently invented the syringe which allowed injections of morphine. By the 1860s the efficacy of locally applied opiates, especially morphine, directly to the skin or nerves for pain relief was widely accepted. The effects of pre – and intraoperative administration of morphine to the area of incision or amputation were investigated. When cocaine became available as a local anaesthetic, owing to the work of Sigmund Freud (Fig 2) and especially, Karl Koller, this soon resulted in its use as a local anaesthetic in diverse procedures (Fig. 3 )
 |  |
Surgical techniques for pain relief represented another great medical advance during the 19th century. With the advent of antiseptic surgery, procedures became less life threatening, allowing investigation of pain relief techniques involving permanent interruption of afferent pathways.
Innovative techniques were developed for treating trigeminal neuralgia, in addition to procedures such as retrogasserian neurectomy and cordotomy, ablation of the sympathetic nervous system, sympathectomy for visceral pain and angina pectoris, and surgical management of neuralgia.
Pain mechanisms
Little was understood about pain mechanisms at the beginning of the 19th century. Many questions such as how sensibility related to movement, whether separate sensory and motor nerves existed, and whether single nerves could perform different functions were still unanswered.
Early researchers tried to explain pain by concentrating on the specialization of functions in different parts of the brain. Investigators such as Claude Bernard, Charles Bell, and Francois Magendie developed innovative experimental procedures that allowed differentiation of sensation from movement and between functions of anterior and posterior spinal nerve roots. A significant impetus to the perception of the nervous system as a system involving the transmission of sensations from the periphery to the centre through a system of complex relays was provided by the work of German physiologist and comparative anatomist Johannes Muller proposed a connection between the anatomic pathway of a fibre and perception of sensation, stimulating further research on specific fibres for pain and nociception.
As a result of such work, an entirely new school of physiologic research was founded. Soon nerve structures were identified in the dermis, leading to investigation of dissociation of sensations in that region, such as sensation of touch, pressure, and pain; and the spinal cord was more realistically appraised as a central processor with the ability itself to affect the transmission of sensations. Other noteworthy contributions were made by Waller, who developed a sectioning technique allowing observation of fatty degeneration of a fibre, leading to an awareness of ascending and descending pathways and the origin of nerve fibres. There were many other pioneers who, through work with patients in pain or self -experimentation, contributed to the general body of medical knowledge:
Weir Mitchell ’s work with neuritis, neuralgia, and causalgia, Henry Head’s discovery of two different types of nerve fibre, and Sherrington ’s notion of an integrated nervous system were major advances establishing a firm foundation for an understanding fibres, which causes central inhibition of pain signals.
Dorsal column stimulators are now an effective means of treating patients with chronic neuropathic and vascular pain. In addition, peripheral nerve stimulators have been used to manage chronic pain after peripheral nerve injury. Deep brain stimulation is a newer technique, still somewhat uncertain in terms of efficacy of pain relief.
New treatment techniques represent another beneficial by product of pain -related research. For instance, the discovery of opioid receptors in the central nervous system provided a rationale for the development of intrathecal and epidural administration of opioids. These now active techniques have resulted in the formation of a new sub -specialty under the umbrella of primary specialists of pain medicine. This subspecialty has been called interventional pain medicine.
Evidence -based medicine is a contemporary movement to establish the most effective algorithms of practice through the use of systematic reviews and meta -analysis. The movement is facilitated by modern global information science, which allows all evidence to be collected and analysed according to standard protocols, which are then disseminated to healthcare providers.
Establishment of interventional pain medicine
Greater understanding of pain mechanisms has resulted in the development of devices offering innovative therapeutic approaches. For instance, dorsal column stimulators were a direct result of the gate control theory. The efficacy of treatment relies on stimulation of low -threshold primary afferent Pain-Relieving Procedures addition, the study of pain has altered the way many physicians manage their patients, increasing awareness of opportunities for alleviating pain and the necessity of early intervention.
Competency and certification of pain physicians
Effective pain management requires that physicians take a multidisciplinary approach to their evaluation, diagnosis, treatment, and rehabilitation of pain problems.
They must not only draw from several medical disciplines, but must also understand the complex nature of pain. This distinction makes pain medicine a unique specialty.
The inadequacy of education in pain management can, and has, led to the poor treatment of pain disorders, especially those of a chronic nature. Although the link between inadequate education and improper treatment is well understood, studies suggest that disparities in pain education continue to exist.
Defining a pain specialist
John Bonica was the first anaesthesiologist who experienced the difficulties of pain management during his years in the army as he was treating the wounded soldiers from the Pacific. He felt strongly that no one particular physician is capable of looking after a patient with pain. He proposed the first concept of multidisciplinary approach to pain management.
What defines a “pain specialist?
Rollin Gallagher stated,
Although pain management is concerned with the diagnosis, treatment, and rehabilitation of a singular sensory symptom, it is essential that practitioners undertake a multidisciplinary approach to achieve these ends. They must also be well versed in the study of pain and its prevention. Although more than 60% of pain specialists originate from the field of anaesthesiology, they can also come from a variety of other disciplines such as interventional radiology, physical therapy, psychiatry, primary care medicine, and neurology. In addition, pain specialists must possess a keen understanding of the variety of conditions and causes associated with pain. This broad range of training and knowledge allows the practitioner to achieve their ultimate goal: the management of a patient’s pain. Despite these extensive requirements, pain management remains classified as only a subspecialty of anaesthesiology under the certification of the American Board of Anaesthesiology .
Present status of interventional pain medicine
Can we, today, looking back over history, state that we have finally conquered pain? The answer has to be the following: in some ways, yes; in some ways, no.
We have certainly conquered surgical pain, the pain of childbirth, and perhaps pain due to trauma. Unfortunately, we have not progressed a great deal in the areas of chronic and cancer pain.
Chronic pain remains a taxing and frustrating situation for both the patient and the clinician. Despite our concern and advanced knowledge, we are still unable to help the patient who comes to us with increasing pain, decreased function, and debilitating psychological difficulties, such as feelings of low self -worth, depression, and inability to cope. One should emphasize the importance of pain management, its advances as a discipline, and the options we now have available to treat a patient with moderate -to-severe pain. The discovery of opioid receptors, a taxonomy of classification of pain, a multidisciplinary multimodal treatment approach, and the establishment of curricula and
training are spectacular advances in pain medicine. It is not surprising, therefore, that these advances have contributed significantly to the practice of medicine. Pain management practitioners must possess a broad skill – set, advanced training and knowledge, and, perhaps above all else, clinical experience. Even so, there remain undeniable disparities in pain management education.
CONCLUSION
A review of the history of pain demonstrates that until the time of Bonica, pain management was considered to be unimodal, unidisciplinary, and managed without any clear structural organization. Today, new drugs and creative techniques and procedures have expanded the scope of pain medicine into a multidisciplinary field of clinical practice. Pain management practitioners must possess a broad skill -set, advanced training and knowledge, and, perhaps above all else, clinical experience. Even so, there remain undeniable disparities in pain management education. Now that we recognize that the problems exist, further efforts must be made by our community to establish and assure clinical reliability and competency in the practice of pain medicine. As pain medicine expands as a subspecialty, so too must educational efforts.
REFERENCES
- Brown, D.L. & Fink, R.B. (2009) The history of regional anesthesia. In Neural Blockade in Clinical Anesthesia and Pain Medicine (ed. Cousins, M. & Bridenbaugh, P.), 4th edition , pp. 1–23. Philadelphia, PA :Wolters Kluwer
- Paradise, L.A. & Raj, P.P. (2004) Competency and certification of pain physicians . Pain Practice 4(3), 235–244.
- Parris, W.C.V. & Johnson, B. (2008) The history of pain medicine .
- In Raj ’ s Practical Management of Pain, 4th edition (ed. Benzon, H.T. ), pp. 3–12. Philadelphia, PA : Mosby .
- Raj, P.P. (1996) Advances in the practice of pain medicine: contributions of pain management. Distinguished Academician 1995 Lecture. Annals, Academy of Medicine Singapore 25(1), 152–159.
- Raj, P.P. ( 2002) Historical aspects of regional anesthesia . In Textbook of Regional Anesthesia (ed. Raj, P.P ), pp. 3–21. New York Churchill
- Raj, P.P. (2010) The 2009 John J. Bonica Award Lecture: the impact of managing pain in the practice of medicine through the ages . Regional Anesthesia and Pain Medicine 35(4),
 |  |  |



