Dr. Bhuvaneswari B
Associate Professor,
Department of Anaesthesiology
AIIMS, Nagpur
Introduction:
Anaesthesia is a medical marvel that has played an indispensable role in alleviating pain and ensuring patient comfort during various medical procedures. One of the most significant advancements in the field of anaesthesia is the development and widespread adoption of regional anaesthesia. The evolution of regional anaesthesia stands out as a remarkable journey that has revolutionized the way surgeries are conducted and postoperative pain is managed.
The Evolution:
Primitive man, seeing in illness and pain the work of evil spirits that had taken possession of the body, tried to get rid of such invaders by methods based on effects on the patient’s imagination. Incantations, charms, amulets, special ceremonies, and faith in the power of medicine men and sorcerers made more or less deep impressions on the subject. In many cases, these methods probably contributed to the alleviation, or even abolition, of pain. From early times, mankind has very often used analogous methods, although the procedures have changed with our supposedly—or perhaps actually— increased understanding of nature and of man himself. Thus, religion has played a role in this connection and still does, to some extent, as well as the personal influence of prominent men (e.g., laying on of hands by kings and prophets). A classic example of the influence of psychic factors in alleviating pain is the well-known story of J. Mesmer (1734–1815) and his pretended use of “animal magnetism” for relieving pain. Hypnosis and acupuncture were the other methods used in different parts of the world for abolishing pain.
Regional anaesthesia was not available when general anaesthesia was first successfully administered in 1846. It had to wait until 1855, when Rynd described the idea of introducing a solution of morphine hypodermically around a peripheral nerve.
The popularization of regional anaesthesia was not possible until two events occurred. First, a local anaesthetic was required, and second, advanced understanding of infectious agents was needed. One of the pioneers of regional anaesthesia was Carl Koller, who, in 1884, introduced cocaine as a local anaesthetic. This breakthrough marked the beginning of a more controlled and less painful era in surgery. Koller’s discovery allowed for specific regions of the body to be numbed, paving the way for countless surgical innovations. The increased understanding of infectious complications was made possible by the introduction of the theories of Lister in the 1870s. The sequence of these requirements was essential in allowing regional anaesthesia to progress since, had physicians progressed to spinal or other regional anaesthetics prior to introduction of asepsis to the practice of medicine, it seems likely that regional anaesthesia would have been significantly delayed or even prevented from progressing into surgical practices.
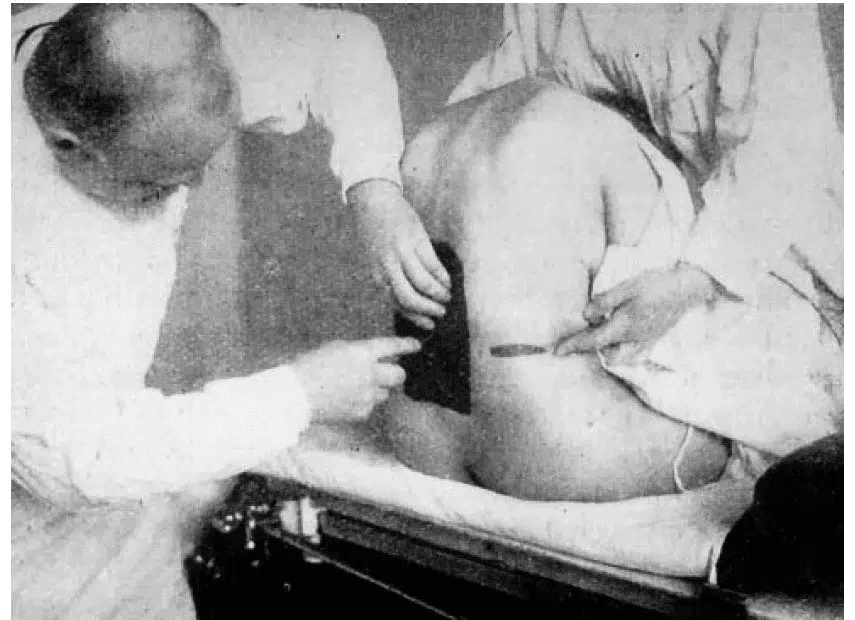
Pic1- Bier performing spinal anaesthesia in 1925.
In the early 20th century, the technique of spinal anaesthesia, or the “saddle block,” was introduced. This advancement allowed for a wider range of surgical procedures to be performed with patients awake, further reducing the risks associated with general anaesthesia.
The revolution:
The 21st century has witnessed a true revolution in regional anaesthesia. Advances in pharmacology and technology have transformed this practice into a cornerstone of modern surgical care.
- Peripheral Nerve Stimulators: From the conceptualization and development of nerve stimulators by Perthes in 1912 to the widespread adoption of the technique of electrolocalization for peripheral nerve blocks in the 1990s, advance research and deeper understanding of nerve-needle relationship led to practice of safer regional anaesthesia by anesthesiologists world over.
- Ultrasound-Guided Techniques: Ultrasound technology has become a game-changer in regional anaesthesia. It allows anaesthesiologists to visualize nerves and the spread of local anaesthetic in real-time, leading to more accurate and effective nerve blocks.
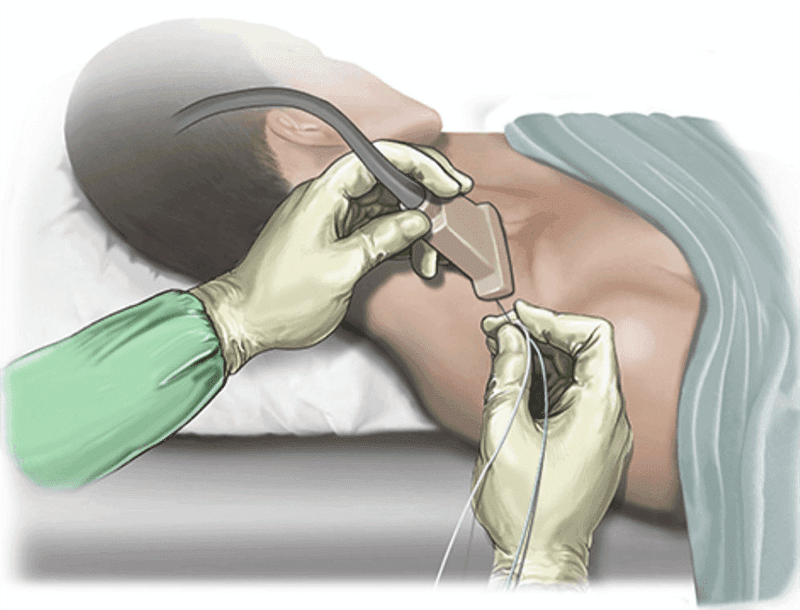
Pic-2 Revolution in regional anaesthesia
- Peripheral Nerve Catheters: Continuous peripheral nerve catheters have extended the duration of pain relief, making them invaluable in post-operative care, particularly beneficial for complex and painful surgeries.
- Multimodal Analgesia: This approach combines regional anaesthesia with systemic analgesics, further enhancing patient comfort and safety.
- Enhanced Recovery After Surgery (ERAS): Regional anaesthesia plays a pivotal role in ERAS protocols. By reducing the need for opioids and minimizing surgical stress, it accelerates post-operative recovery and reduces complications.
- Patient-Centred Care: Anaesthesiologists now tailor regional anaesthesia to each patient’s unique needs. Individualized treatment plans improve patient comfort and satisfaction, leading to better overall surgical experiences.
- Social-Media: The advent of social media has revolutionised the world of regional anaesthesia by facilitating global interactions, content curation and lifelong learning, research dissemination, and enhancement of the traditional conference experience.
Regional anaesthesia offer:
- Improved pain management
- Lower complication rates
- Faster recovery
- Enhanced safety
Conclusion
Regional anaesthesia has evolved from ancient practices to a modern revolution. As we continue to embrace innovation and individualized care, the future of regional anaesthesia looks promising. Regional anaesthesia has come a long way, and its journey is far from over.



